This project was led by Yiqing Xia and Huiting Ma, and published in the International Journal of Infectious Diseases. The work was funded by a Canadian Institute of Research grant.
Why did we conduct this study?
The COVID-19 pandemic has strained hospital and health care systems. Understanding patterns of hospital surges with COVID-19 and deaths among those who are hospitalized can help us anticipate changes in hospital demands, and better plan for and allocate healthcare resources.
What did we do?
We used population-based data on COVID-19 hospitalizations in Ontario and Québec to describe trends in risk of death and length of stay in hospital (in general) and in intensive cares units (ICUs) due to COVID-19 across three waves of the pandemic (March 2020 to May 2021). We accounted for other factors that may influence these outcomes, such as: individual demographic characteristics (e.g., age, sex, residence in a long-term care home, vaccination status), COVID-19 characteristics (e.g., variants of concern), and hospital characteristics (e.g., patient load in hospital, facility type).
What did we find?
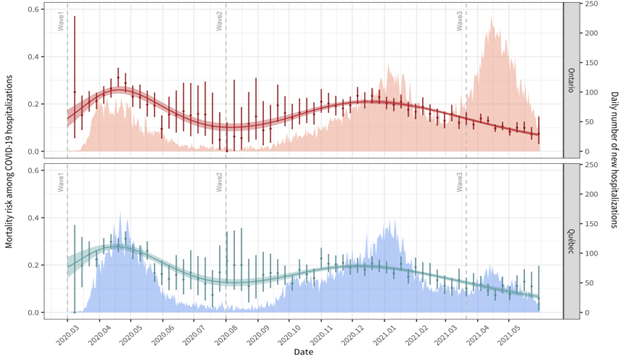
We identified 26,541 hospitalizations from Ontario, and 23,857 hospitalizations from Quebec in the first 3 waves of the pandemic. We found that the risk of death with COVID-19 in hospital peaked in the first wave of the pandemic at 31%, and was lowest in the third wave of the pandemic at 6-7%. After adjusting for other factors, trends in risk of COVID-19 death did not change. Variants of concerns were associated with increased in-hospital mortality. Hospital mortality was also higher when the patient load in hospitals was higher. Overall, the lengths of stay in hospital and in ICUs decreased over the course of the first 3 waves.
What do these findings mean for our healthcare systems?
- In-hospital mortality declined over the course of the pandemic’s first three waves even after accounting for other factors, suggesting improvements to clinical care and treatments may have played a role.
- The association between higher patient load and in-hospital mortality highlights the vulnerability of patient care during hospital surges. The findings signal the importance of health systems preparedness with adequate and adaptive systems-level buffers (health and human resources) in order to minimize downstream negative effects on patients.
