This paper is published in CMAJ.
Why did we conduct this study?
Understanding inequalities in COVID-19 transmission along social determinants of health could help develop effective mitigation strategies that are tailored to local pandemic transmission contexts. However, few studies to date have quantified and compared the geographical concentration of COVID-19 cases by social determinants across cities in Canada, and the extent to which the magnitude of inequalities might vary between cities and provinces.
What did we do?
We worked with researchers across Canada to carry out this study. We quantified social determinants based on the geographic concentration of COVID-19 cases across 16 cities (defined as metropolitan areas) in four Canadian provinces (British Columbia, Manitoba, Ontario, and Québec).
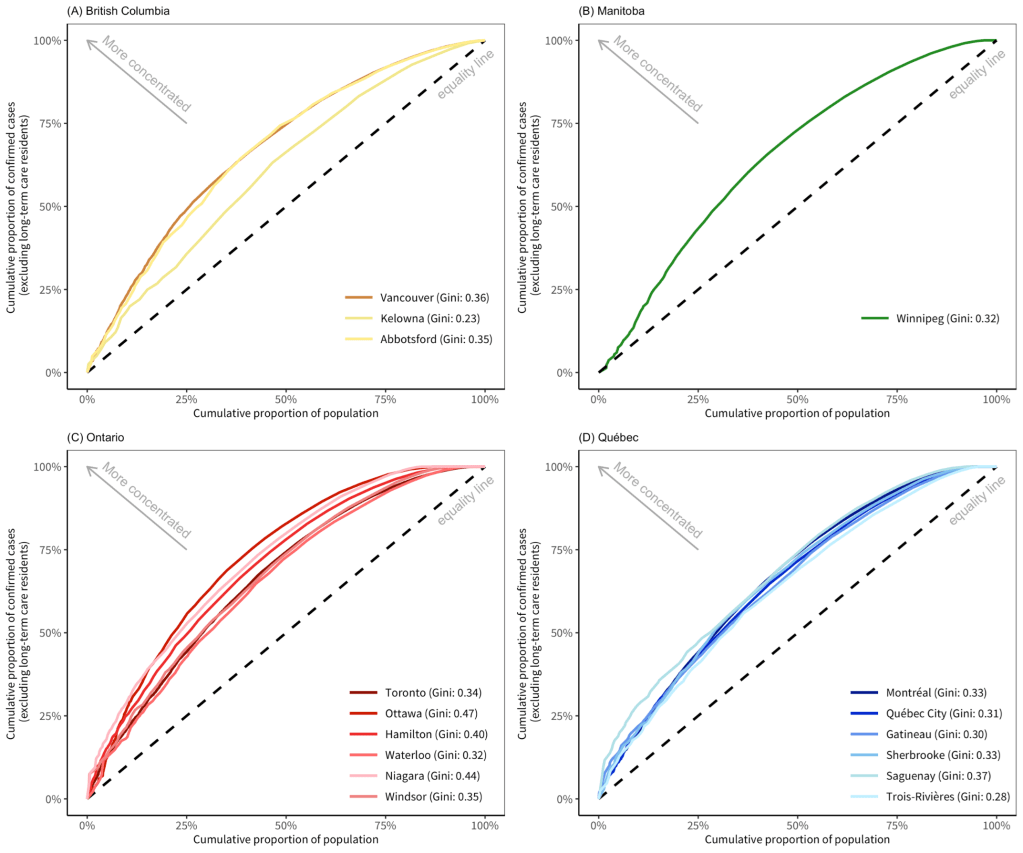
Gini coefficients were calculated and Lorenz (concentration) curves were used to visualize the differences in risk of COVID-19 infection by:
- socio-demographic indices (income, education attainment),
- proxies for systemic racism (proportion visible minority, proportion recent immigration),
- dwelling-related indicators (proportion not living in high-density housing), and
- occupation-related variables (proportion working in essential services).
What did we find?
The greatest geographical concentration of cases was found in cities in Ontario, followed by British Columbia, Manitoba, and Québec.
Cases were disproportionately concentrated in areas with:
- lower income,
- lower education attainment,
- higher proportion of visible minorities,
- higher proportion of recent immigrants,
- higher proportion of high-density housing, and
- higher proportion of essential workers.
A consistent feature across cities was the concentration of cases by proxies for systemic racism (proportion visible minority). However, the magnitude of concentration by social determinants varied across metropolitan areas.
What do these findings mean?
There are two important implications of the findings:
- Prioritizing and allocating resources to geographical hotspots (areas with disproportionate concentration of cases) could lead to a more effective and efficient response, and reduce inequalities, especially in the context of limited resources.
- Cities may differ with respect to which determinants were most associated with geographical clustering of COVID-19 cases. Each city would therefore benefit from tailoring its geographically-prioritized strategy to its local structural determinants affecting risk of acquiring COVID-19 infection.
As such, geographically-prioritized allocation of resources and services that are tailored to the local mediators of inequalities in acquisition and transmission risk of COVID-19 should be considered – such as vaccination programs, outreach access to testing and wrap-around support for isolation and quarantine, and access to early treatment.
This research was led by Yiqing Xia and Huiting Ma, and funded by the Canadian Institutes of Health Research.