This work was led by Ph.D. candidate Jesse Knight with Sharmistha Mishra and our close collaborator Darrell Tan. The work was supported by the Natural Sciences and Engineering Research Council of Canada (NSERC) doctoral award and the University of Toronto Emerging and Pandemic Infections Consortium (EPIC) MPXV Collaborative Rapid Research Response. The paper is published in CMAJ.
Why did we conduct this study?
During the first few weeks of mpox (formerly monkeypox) spread in Canada, it was not clear exactly how many vaccine doses would be available, or when. Many public health practitioners and members of the hardest-hit GBMSM community (gay, bisexual, and other men who have sex with men) were interested to know how best to distribute a limited number of vaccine doses between Canadian cities.
What did we do?
We created a simple simulation model of mpox transmission and vaccination among GBMSM within two partially-connected cities (that themselves represent partially-connected networks). We then varied the modeled characteristics of the two cities, including the city size, each city’s epidemic potential (reproduction number “R0”), the connectedness of the cities, and how many cases were initially imported into each city. For each set of city characteristics, we calculated the “optimal” distribution of 5000 vaccine doses between the two cities, as that which minimized total infections after 90 days.
What did we find?
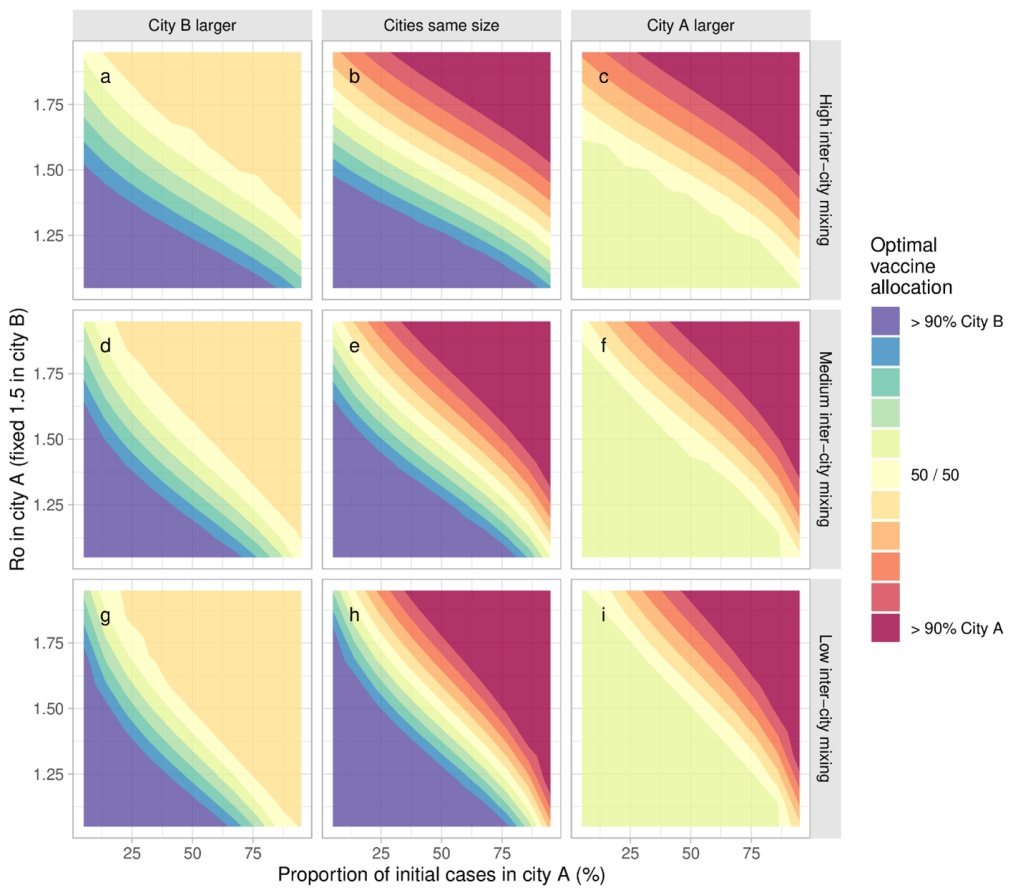
Under our modeling assumptions, we found that a limited number of vaccine doses could generally minimize infections when prioritized to – the larger city, the city with a bigger R0, and/or the city with more initial cases. More connectedness between cities made the R0 of each city more important, and the initial cases less important. When characteristics were “mixed” (for example, one city had a larger R0 but fewer initial cases) then the optimal distribution included doses shared between the two cities (Figure).
What do these findings mean?
Our modeling study helps show how city-level characteristics can be used to optimize vaccine distribution during an emerging epidemic. We also highlight the importance of estimating key city characteristics – like epidemic potential (R0) and connectedness to other cities – quickly, and ideally even before an outbreak occurs based on reasonable assumptions.